On this page

Community Paramedicine is an evolving model of community-based health care in which paramedics operate in an expanded role, outside traditional emergency response and transport. The program aims to support individuals to access collaborative resources in order to reduce dependency on 911 and possible transports to the emergency department.
Main goals of community paramedicine
- Reduce the number of repeat emergency medical services calls
- Reduce the number of low acuity patients in the emergency department transported by paramedics
- Enable vulnerable/at risk individuals and older adults to live safely in their own homes and reduce the use of more costly care, such as acute care hospitals and long-term care
Other benefits
- The right service at the right time to the right client
- Complete the client’s “wrap-around” care
- Improve client care and system coordination
- Process development to ensure patient is connected to best-suited resource for assessment and service provision
- Collaboration, partnership development amongst stakeholders
- Improve health outcomes for high risk, vulnerable seniors in the community
- Process development for managing crisis mental health issues
Community Paramedicine services
Referrals to community resources
In the course of responding to a 911 call, any paramedic can submit a formal referral to a partner agency for additional assessments on behalf of patients with unmet needs having received the patient’s consent. All patients can be referred regardless of whether they are transported to hospital or not.
Community Paramedic home visit
There are several occasions when a home visit is conducted:
- Paramedic referrals occur whenever the patient gives consent. However, if refused, the referral is transferred to the Community Paramedicine coordinators who will visit the patient’s residence to address the concern.
- The patient is a shared client with another agency/community partner. The community paramedic is asked to visit the patient to reduce duplication of assessments.
- Clients that are considered as high 911 users.
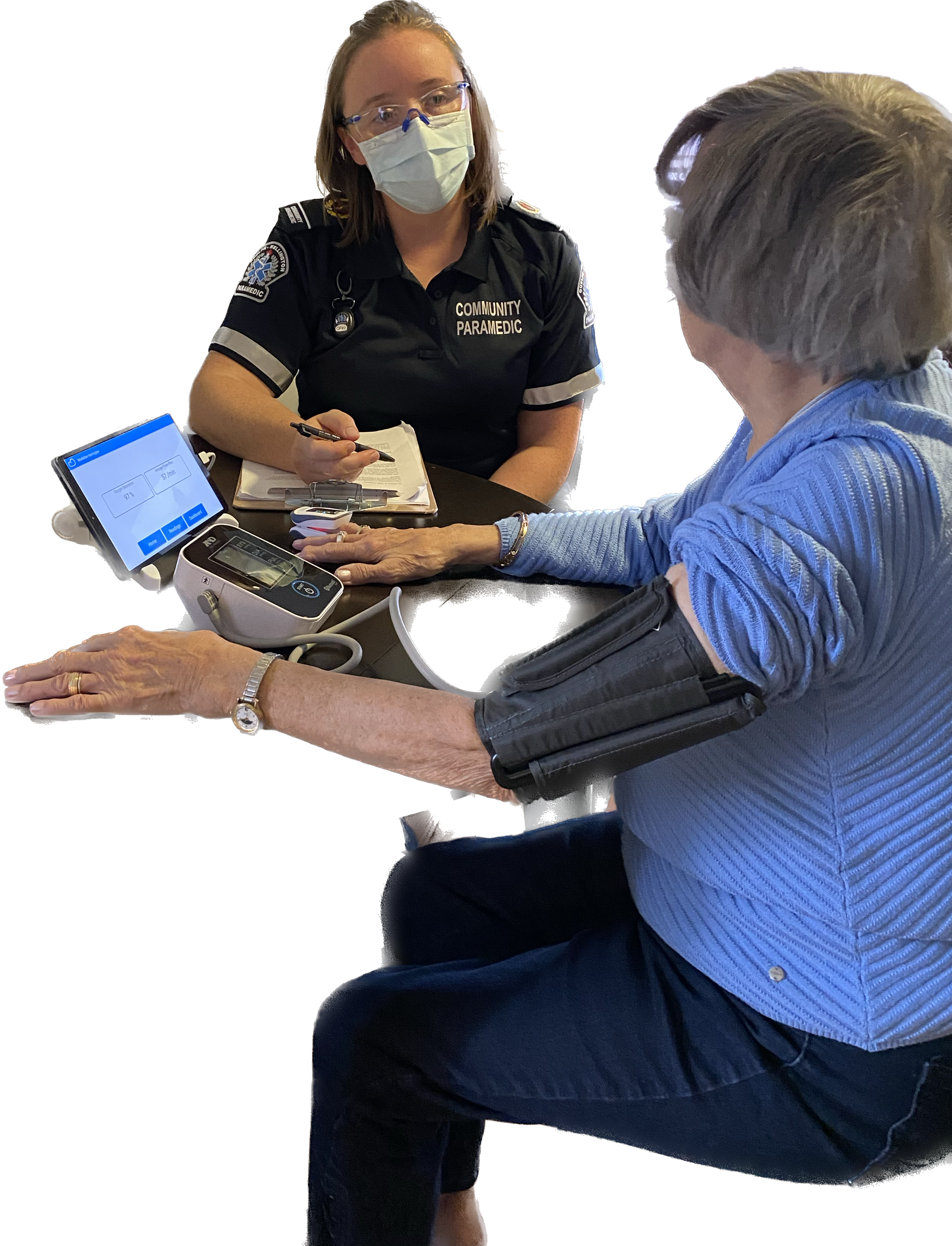
Community Paramedic at clinic
Community Paramedic Health Clinic: Researchers from McMaster University in partnership with Guelph-Wellington Paramedic Service are working together to host clinics in buildings identified by Wellington Social Housing with focus on the prevention of chronic conditions, predominately high blood pressure, diabetes mellitus, cardiovascular disease risk, and to reduce the risk of falls, in mostly older adults living in subsidized housing. Older adults are more at risk of developing cardiovascular disease, diabetes and experiencing falls which can lead to 911 emergency calls resulting in expensive emergency room visits.
Community Paramedic Remote Care Monitoring
People that suffer from congested heart failure (CHF), diabetes (DM) and/or chronic obstructive pulmonary disease (COPD) will have their biometric readings monitored remotely through technology, to recognize exacerbations and trends to improve patient’s health awareness and decrease dependency on emergency services and hospitals admissions.
Public Access Defibrillator loaner program
The general public may borrow an automated external defibrillator (AED), at no cost, for short-term community and family events within the city of Guelph and county of Wellington.
File of Life (fridge magnet)
The File of Life program is meant to provide quick and easy access to basic medical information to first responders if an individual is unable to provide the information themselves. It is a magnetic folder that can be easily kept on the refrigerator for speedy access in the event of an emergency. It includes personal information, medical conditions, medications and allergies. Request a File of Life via email or download one in one of the 5 available languages:
- Mandarin – File of Life (PDF)
- Punjabi – File of Life (PDF)
- Italian – File of Life (PDF)
- English – File of Life (PDF)
- French – File of Life (PDF)
Referral forms
Community Support Services and Primary Care Providers may fax in a referral form, for any client.
Community Paramedic Referral form (PDF)![]() eReferral via Ocean
eReferral via Ocean
For more information
Guelph-Wellington Community Paramedicine
Public Services, Emergency Services
Office: 519-822-1260, extension 3379
Email: [email protected]
Fax: 519-840-2565
Twitter: @gwps_cp
![]() Also available on Hypercare: search ‘paramedic’
Also available on Hypercare: search ‘paramedic’
